|
Periodontal disease is an infection of the oral tissues that support the teeth in place. It is mainly the result of inflammation and infections that occur around the gums and bones that support the teeth. It occurs when a sticky film of bacteria called plaque builds up, persists, and hardens into tartar or calculus. Over time, plaque can spread and grow below the gum line, and release toxins that stimulate a chronic inflammatory response. At this point, only a dental health professional is able to safely remove the tartar and stop the periodontitis process. The body’s immune system essentially turns on itself in an attempt to fight the bacteria. The toxins and the body’s enzymes meant to fight infections will start to break down bone and connective tissue that secure the teeth in place. In turn, the inner layer of gum and bone is separated from the teeth, forming pockets and space to collect debris. With the progression of the disease, the pockets deepen as more tissue and bone are destroyed, no longer anchoring the teeth in place and causing them to be loose, fall out, or need to be removed professionally. The diagnosis of periodontal disease is classified by stage and grade. Stages range from initial to severe and describe the acuteness of the disease. The grade communicates the rate of progression and determines the anticipated treatment response. Periodontal disease is common in the United States and is specifically prevalent among adults. Reports from the Centers for Disease Control and Prevention (CDC) found the following statistics regarding periodontitis in the United States:
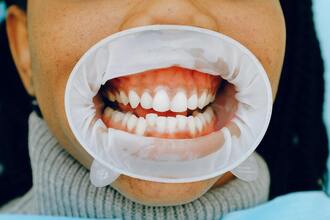
PERIODONTAL DISEASE SYMPTOMSPeriodontitis can be difficult to identify for the untrained eye. However, symptoms increase in severity as the disease progresses:
WHAT IS GINGIVITIS?In its early stages, periodontitis is known as gingivitis. Gingivitis is the inflammation of the gums caused by the build-up of bacteria in plaque. Over time, the bacteria release acids that attack the teeth’s enamel and lead to decay. Plaque hardens into tartar after 72 hours, lining the gums, and making it difficult to clean the teeth and gums without professional intervention. The buildup irritates and inflames the gums over time, causing gingivitis. Gingivitis is common with most people experiencing it at some point in their lives. However, the mild symptoms and little to no discomfort make it easy to ignore, leading to a more destructive oral disease. With gingivitis, no irreversible damage to the bones or tissue has occurred and the teeth are still firmly planted in their sockets. To the untrained eye, this disease is subtle and difficult to identify as a risk. However, during this stage, the gums are red, sensitive, swollen, and easily bleed when touched. Gingivitis is reversible and can be prevented and treated by brushing and flossing every day along with regular dental checkups and cleanings. If left unchecked, gingivitis can develop into periodontitis or lead to other long-term consequences. RISK FACTORS OF GUM DISEASEGingivitis and periodontal disease are typically caused by poor oral hygiene–poor brushing and flossing habits that allow tartar to form on the teeth. However, other risk factors include:
PREVENTION AND TREATMENT FOR GUM DISEASEDaily oral hygiene and routine dental exams are key when it comes to gum disease prevention. Brushing twice a day with fluoride toothpaste paired with regular flossing helps to remove plaque between teeth. Special toothbrushes, toothpicks, or water flossers are recommended. More severe forms of periodontitis require more extensive treatment, such as deep cleanings below the gum line, medications, or corrective surgery. Both immediate and long-term care is necessary for treating periodontal disease. The dental professional will evaluate and determine the best course of action. Scaling and root planing is a common method of treatment. It is a more intensive version of cleaning and is aimed to remove plaque and tartar above and below the gum line. Tartar is removed from the tooth’s surface and crown, and the root surfaces are also smooth to prevent bacteria from collecting. In addition, laser therapy or antibiotics may be recommended. Extra monitoring, routine cleanings, and dental visits may be required as well. Those with severe decay and periodontitis will need to undergo surgery. Again, the dentist will determine the long-term plan for maintaining good oral hygiene post-treatment. Sources: Periodontal Treatment Periodontal Disease Periodontal (Gum) Disease Gingivitis and Periodontal Disease (Gum Disease) Gum Disease Information Keywords:
The Dental Lab, gum disease, periodontitis, periodontal disease, gingivitis, gums, tartar, plaque, teeth, tooth
0 Comments
Leave a Reply. |